

The SCENIHR opinion states:
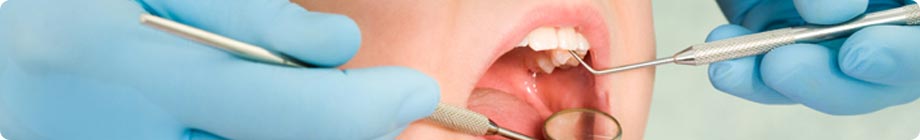
3.3.3. Mercury toxicology
In general, the toxicology of mercury is highly dependent on the route of administration, the exposure conditions and the speciation of the mercury. Since human exposure to mercury from dental amalgams may occur by inhalation of mercury vapour released from the dental fillings into the oral cavity, by ingestion of the released elemental mercury, or swallowing small pieces of amalgam releasing elemental mercury in the alimentary tract, this discussion focuses on the toxicology of elemental mercury.
3.3.3.1. Toxicokinetics
Oral ingestion of elemental mercury results only in a very limited absorption, typically < 0.01 % of the dose (ATSDR 1999, MAK 1999, Klaassen 2001). Dermal absorption of liquid elemental mercury is also very limited. In contrast, approximately 80 % of the inhaled elemental mercury is absorbed in the lungs. Due to the high lipid solubility, elemental mercury rapidly penetrates alveolar membranes and is then distributed to all tissues of the body. Elemental mercury is slowly oxidized in the blood in a saturable process to give Hg2+, probably by catalases. Due to the ease of saturation of the enzymatic oxidation of elemental mercury to Hg2+, the proportion of elemental mercury in blood increases with increasing dose of elemental mercury. A small part of the elemental mercury dose received is also eliminated by exhalation and a small part of the dose is also delivered to the central nervous system. Oxidation of elemental mercury may also occur in the central nervous system and result in an accumulation of Hg2+ in the central nervous system since Hg2+ is unable to cross the blood-brain barrier and diffuse out of the brain. Hg2+ is tightly bound to sulphydryl groups in proteins which represents the principal mode of action for its toxicity and is responsible for the slow elimination from the organism. It may be eliminated by excretion within urine and/or faeces. The elimination of elemental mercury or Hg2+ follows complex kinetics with half- lives in the range of 20 - 90 days. Usually, the kidney contains the highest concentration of mercury following exposure to elemental mercury and Hg2+. After repeated exposures, a steady state level of blood mercury is reached, this being influenced by the average intake of mercury. At the end of the exposure, mercury levels slowly decline.
3.3.3.2. Toxicity of Elemental Mercury
Due to the very low absorption of elemental mercury after oral intake, this section focuses on toxic effects observed after inhalation of elemental mercury. Due to the widespread use of mercury in industrial settings, a large and detailed database on human effects of elemental mercury inhalation is available. A number of reviews addressing the toxicity of elemental mercury have been published (MAK 1999, BAT 1997, UNEP 2002, ATSDR 1999, IRIS 2002)
The assessment of elemental mercury toxicity is mainly based on observations in occupationally exposed humans. Inhalation of extremely high concentrations of elemental mercury, in excess of 10 mg/m3, may produce bronchitis and pneumonia, in addition to symptoms of the central nervous system. However, such concentrations are many orders of magnitude above those encountered through the release of elemental mercury from dental fillings. After long-term elemental mercury exposure in occupational settings, and under occupational hygiene conditions considered as poor by present standards, the major effects of elemental mercury reported are on the central nervous system. The major manifestations of mercury poisoning from inhalation of elemental mercury are increased excitability and tremors. Characteristic symptoms after long-term high dose exposures (the inhalation of concentrations above 0.5 mg/m3 for many years) are muscle tremors in fingers, eye lids and lips, which may progress to chronic spasms of the extremities. Early signs of toxicity after inhalation of mercury are less specific and the early phase of toxicity is often referred to as “micromercurialism”. Clinical findings in this condition are tremor, enlargement of the thyroid, increased uptake iodine in the thyroid, tachycardia, gingivitis and haematological changes. For diagnosis of the early phase of elemental mercury intoxications, at least three of these findings should be present along with increased mercury concentrations in blood or increased mercury excretion with urine. After chronic occupational exposure to mercury vapour, proteinuria and even a nephritic syndrome have been described in humans. The glomerular damage may progress to an interstitial immune-complex nephritis. Gingivitis and hypersalivation with a strong metallic taste are considered to be further symptoms of chronic inhalation exposure to elemental mercury.
Quantitative data on elemental mercury inhalation exposure, mercury concentrations in blood and urine and early effects of mercury toxicity have been established. The non- specific symptoms of micromercurialism are observed at long term exposures to elemental mercury air concentrations of 0.05 mg/m3, or at concentrations of mercury of 35 µg/l in blood or 150 µg/l in urine. Overt neurotoxicity (tremor) occurs after long term inhalation of elemental mercury at concentrations between 0.1 and 0.2 mg/m3 with resulting blood mercury concentrations between 70 - 140 µg/l and urinary mercury in the range of 300 - 600 µg/l (MAK 1999, BAT 1997, UNEP 2002, ATSDR 1999, IRIS 2002).
Occupational allergies to mercury were rare in the past, even with widespread exposures to elemental mercury at the workplace and the use of mercury in medicinal preparations (including the use of Hg2+ due to its bactericidal activity) and consumer products (Kanerva et al. 1993).
Regarding animal toxicity studies, no adequately performed studies with elemental mercury inhalation are available for evaluation. However, long term oral administration of Hg2+ to rodents causes glomerulonephritis, which was found to have an immune basis, thus being similar to the human disease described after long term elemental mercury inhalation (Bigazzi 1999, Havarinasab and Hultman 2005, Havarinasab et al. 2007). Mercury compounds are well known for their immunosuppressive activity (Havarinasab and Hultman 2005). Organic mercury compounds such as methylmercury and ethylmercury are much more potent suppressors of the immune system than inorganic mercury or elemental mercury. In a susceptible genotype of mice, inorganic mercury interacts with the immune system inducing immunostimulation, antinuclear antibodies and systemic immune-complex deposits, a syndrome designated as mercury-induced autoimmunity (Hultman et al. 1989, Reuter et al. 1989). In mice a similar effect was observed for mercury vapour (Warfvinge et al. 1995). In a genetically modified mercury susceptible rat model for autoimmune diseases, the Brown Norway (BN) rat, dental restorations with amalgam induced immune activation with an increase in IgE plasma concentrations, and immune complex deposits in systemic organs including the kidney, whereas this was not observed in BN rats receiving composite resin restorations, or mercury resistant Lewis rats (Hultman et al. 1998). Another model for studying mercury induced autoimmunity is the New Zealand White rabbit in which mercuric chloride treatment results in immune deposits in kidneys and other organs (Roman-Franco et al.1978)
3.3.4. Toxicology of other metallic elements in amalgam
3.3.4.1. Toxicology of silver
Despite the widespread use of silver and silver ions in industry and for medicinal purposes, only limited information on silver toxicity is available. Silver exposure is ubiquitous in the general population and dietary intake is estimated at 70 - 90 µg/day. Silver ions may be absorbed from the gastrointestinal tract after oral uptake or after inhalation of silver containing dusts. At higher local concentrations, silver ions may produce skin and gastrointestinal tract irritation. The critical effect of excessive silver absorption is argyria, a deposit of silver sulphide resulting in local or generalized impregnation of tissues. Other specific toxic effects of silver in humans or in experimental animals have not been described. Silver does have antimicrobial activity (Drake and Hazelwood 2005).
3.3.4.2. Toxicology of copper
Copper is an essential nutrient that is incorporated into a number of metalloenzymes. Symptoms associated with copper deficiency in humans include anaemia and leucopoenia. Copper released from dental amalgams may be readily absorbed from the stomach and small intestine. After nutritional requirements at the recommended daily intake are met (2 mg/person), excess copper (well above TDI of 0.5 mg/kg bw/day) is absorbed into gastrointestinal mucosal cells and into the liver induces the synthesis of and binds to metallothionein. Bound copper is excreted when the cell is sloughed off or released into bile and excreted in the faeces. Exposure to excessive levels of copper can result in a number of adverse health effects including liver and kidney damage, anaemia, immunotoxicity, and developmental toxicity. One of the most commonly reported adverse health effect of copper in humans is nausea, vomiting, and/or abdominal pain. The observed effects are not usually persistent and gastrointestinal effects have not been linked with other health effects. The liver is also a target of toxicity. Liver damage has been reported in individuals ingesting lethal doses of copper sulphate. Liver effects have also been observed in sensitive subpopulations such as individuals diagnosed with Wilson’s disease or Indian childhood cirrhosis, or idiopathic copper toxicosis. These syndromes are genetic disorders that result in an accumulation of copper in the liver or with excessive copper exposure. Inflammation, necrosis, and altered serum markers of liver damage were observed in rats fed diets with copper sulphate levels that are at least 100 times higher than the nutritional requirements (Klaassen 2001).
3.3.4.3. Toxicology of tin
Humans chronically exposed to inorganic tin (e.g., stannic oxide dust or fumes) manifest a benign form of pneumoconiosis known as stannosis, which mainly involves the lower respiratory system. Gastrointestinal effects, such as nausea, vomiting, and diarrhoea have been reported in subjects ingesting food items containing inorganic tin. Based on the available studies in humans, there is no evidence that inorganic tin affects reproduction or development in humans or that it is neurotoxic, mutagenic, or carcinogenic. Studies in animals have not clearly established potential target organs for inorganic tin toxicity. Of the effects described, signs of anaemia and gastrointestinal distension appear to be tin-related. No adverse reproductive or developmental effects of inorganic tin were reported. Studies in animals have shown that excess dietary tin reduces serum iron and copper levels. Excess doses of tin affects the metabolism of other metals such as copper, zinc, and iron. Due to the altered disposition of these metals, it is difficult to ascertain whether an effect is specific to tin itself or is due to fluctuations in tissue levels of other metals. Feeding a diet with excess tin to rats produced signs of anaemia and individuals with low levels of iron or copper may be at risk of developing signs of anaemia if they consume excessive amounts of tin. (Klaasen 2001).
3.3.4.4. Toxicology of zinc
Zinc is an essential nutrient and zinc deficiency has been associated with dermatitis, anorexia, growth retardation, poor wound healing, impaired reproductive capacity, and depressed mental function; an increased incidence of congenital malformations in infants has also been associated with zinc deficiency in the mothers. Nausea has been reported in humans exposed orally to high doses of zinc chloride. Other gastrointestinal symptoms reported in cases of excess zinc exposure include vomiting, abdominal cramps, and diarrhoea. The limited data suggest that single-dose exposures in the range of 140 - 560 mg zinc are sufficient to cause these effects, which are consistent with gastrointestinal irritation. Following longer-term exposure to doses of 0.5 - 2 mg zinc/kg/day, the observed symptoms are indicative of copper deficiency. The most noticeable manifestation of the decreased copper levels due to the interaction with zinc is anaemia, manifesting as decreased erythrocyte number. Long-term consumption of excess zinc may also result in decreased iron stores. Effects of zinc on reproductive or developmental end points have been noted in oral-exposure animal studies, but generally only at very high doses (>200 mg/kg/day) (Klaasen 2001).
3.3.4.5. Conclusions
The elements other than mercury contained with dental amalgam all have their own, different profiles in terms of essentiality and/or toxicology. There is no scientific evidence that any of those elements currently used in dental amalgam restorations constitute a risk of adverse health effects in individuals apart from allergic reactions to the individual elements.
3.3.5. General conclusions concerning correlation between exposure and toxicology (risk assessment)
A number of regulatory limits for mercury exposures have been set by various organisations. When using these regulatory limits describing safe intakes of mercury (safe as defined to be without toxic effects after lifetime exposure) it should be recognised that many of the values are recommended for dietary intake of mercury ions and methyl mercury. Therefore, these limits have only limited use for the assessment of mercury emissions from dental amalgams since the exposure in this case is inhalation or ingestion of elemental mercury. Due to the differences in toxicokinetics as outlined above, the assessment for mercury exposure from dental amalgams therefore should be based on resulting blood levels of mercury and/or urinary excretion of mercury. Toxicologically based limits for both of these media have been developed.
Due to the small dose received by inhalation of mercury from amalgams, a direct comparison of maximal mercury air concentration in the oral cavity of individuals with amalgam fillings and occupational limits for air concentrations of mercury requires consideration of absorbed dose. As shown in table 1, inhalation of mercury at the occupational exposure limit results in an uptake of more then 300 µg of Hg per day, whereas inhalation of mercury from dental amalgams gives body burdens which are at least 20 fold lower then those resulting from occupational exposures at present limits for air concentrations.
Based on the evaluation of several longitudinal studies involving blood samples to determine mercury content over a prolonged time period, the German MAK-Commission (tasked to set occupational exposure limits which are without health risks) concluded that even many years of mercury exposure to concentrations that result in urinary mercury levels of 100 µg/l or even higher do not cause objective adverse effects. The urinary mercury levels were equivalent to mercury concentrations in blood of approximately 23 µg/l. The BAT-value (maximal permissible concentration of hazardous compounds or their metabolites in body fluids) was therefore set at 100 µg/l of urine or 25 µg/l of blood and is considered a No-adverse-effect-concentration for mercury in humans.
For the general population, the Federal Environment Agency (Umweltbundesamt (UBA)) derived reference values including general background exposure to mercury from various sources (fish and seafood consumption, mercury in other foods) of 1.4 µg/l of urine and of 2 µg mercury/L of blood in adults without amalgam fillings and with low seafood consumption. According to UBA, no adverse effects of mercury are observed at blood levels lower than 5 µg/l (including pregnant women) and urinary mercury concentrations lower than 0.7 µg/l. These assessments included both inorganic mercury and the more toxic methyl mercury (UBA 1999).
Table 2 gives respiratory air concentrations, blood levels and urinary excretion of mercury in individuals with amalgam fillings and compares these to levels of mercury considered safe for occupational exposures. It is clear that, although exposure to individuals with amalgam restorations does occur, the levels of exposure encountered as between 5 and 30 times lower than those permitted for occupational exposure.
Source & ©: SCENIHR,
![]()
The SCENIHR opinion states:
3.3.6. Adverse effects in individuals with amalgam restorations
Mercury toxicity associated with methylmercury, elemental and inorganic mercury is well documented (see above). The question remains, however, whether metallic mercury exposure from dental amalgams is the cause of adverse health effects, including multiple sclerosis, autism, CNS and renal damage, chronic fatigue, memory impairment and depression. These conditions and their etiology have been studied extensively and risk factors are well defined (see the review article by Brownawell et al. 2005).
The parameters of the adverse effects may be toxicological, allergic and/or psychological.
3.3.6.1. Localized mucosal reactions
The possibility that restorative dental materials could be responsible for lesions within the mouth associated with direct contact between the material and the oral mucosa is obviously of importance. Such localised reactions are often discussed in the context of allergies and hypersensitivity.
In the dental clinic two reaction patterns are relevant: the delayed reaction (Type IV) and the immediate reaction (Type I). In the type IV reaction, the incomplete allergens (haptens) are brought in contact with tissue proteins by way of the oral mucosa to form complete allergens. Provided that previous sensitisation has taken place, specialised T- lymphocytes now produce inflammatory mediators causing tissue damage, seen as contact mucositis, i.e. intra-oral diffuse, red zones, blisters, or ulceration with pain and burning sensation. The inflammation is not always limited to the exposure site. Contact dermatitis may be observed in the face or more distant locations as urticarial or eczematous reactions. A suspected Type IV reaction may be confirmed with an epidermal patch test (see standard textbook such as Roitt and Delves 2006)
An immediate type (Type I) allergic reaction is based on the release of vasoactive humoral mediators from mast cells or basophilic granulocytes. These mediators are released from the cells upon contact with antigens binding to the IgE antibodies on their surface. The antigen specific IgE antibodies provide the specificity of the allergic response. The released mediators lead to increased capillary permeability and contraction of smooth muscles. The symptoms may consist of urticaria, asthmatic seizures, swelling of the mucosa of throat and eyes and even result in anaphylaxis, all seen within minutes. This immediate type hypersensitivity is in general associated with allergic responses to protein allergens. Potential full allergens encountered in restorative dentistry are mainly limited to the accessories used, including residual proteins from natural rubber latex in gloves, rubber dam, polishing remedies or parts of anaesthetic cartridges.
A chronic inflammatory response of the gingival tissue around restorations may be present, which appears as chronic gingivitis, recurrent necrotic gingivitis and periodontal pockets. When patients with self-diagnosed oral problems (142 women and 76 men) were examined, the mean concentration of mercury in the whole blood was 17.3 nmol/l and no value exceeded 50 nmol/l. Mental disorder was diagnosed in 93 cases (42.7%), including 41 cases of generalized anxiety disorder and 12 cases of panic disorder. A total of 82 patients (40%) did not work because of medical reasons or unemployment (Herrstrom and Hogstedt 1993). However, no correlation could be demonstrated between the oral symptoms and a generalized toxic effect of amalgam fillings.
Amalgam tattoos, which are occasionally observed, are associated with the iatrogenic introduction of small particles of dental amalgam, inadvertently implanted into oral soft tissues during dental procedures. Tattoos are resistant to protracted conventional therapies. Most of the foreign bodies examined by light and EDAX methods contained amalgam (amalgam dusts) that appears either as fine granular or larger globular structures implanted in gingival tissues. There is no free mercury, but large globular pieces of amalgam, which induce metallothionein expression in adjacent histiocytes. There is no consequence to the presence of tattoo, except the unpleasant dark blue staining of the gingiva (Lau et al. 2001) and currently there is no indication for the surgical removal of these tattoos.
Metals in close contact with skin and mucosa are well-recognized causes of contact dermatitis including mercury (Garner 2004). Oral lichen planus is associated with dental restorations and one of the causes may be contact allergy to constituents of dental amalgam. Khamaysi et al. (2006) examined 134 patients presenting with mucosal reactions, where the most frequent oral manifestations were cheilitis, peri-oral dermatitis, burning mouth, lichenoid reactions and orofacial granulomatosis. Patch testing showed several allergens in this group, including metals such as gold, cobalt, platinum, nickel and mercury. No specific association between any one metal and a specific clinical manifestation was found but mercury was not a significant factor contributing to the pathogenesis of oral lichenoid reactions.
When dental amalgam was removed in a subgroup of patients suspected of amalgam contact hypersensitivity lesions, considerable improvement was seen (Thornhill et al. 2003) Seventy percent of these patients also showed a positive skin patch test for amalgam or mercury. Total or partial replacement of amalgam fillings following a positive skin patch test reaction to ammoniated mercury, metallic mercury, or amalgam is followed by significant improvement, when the lesions are confined to areas in close contact with amalgam fillings. Even if there is no topographic relationship, improvement occurs in nearly all patch test-positive patients (Laeijendecker et al. 2004). If mercury is the allergen, the removal of the filling should lead to complete remission after about 3 months. A total of 51 patients who had oral lichenoid lesions suspected to be related to the dental restorations were investigated. Fifty three per cent (n= 27) of the patients had positive patch test reactions, 24 of them for one or more mercury compounds. Nine months after the removal of the fillings, 42% of the patients were completely healed. Improvement was found in 47% especially when lesions were in close contact with restorations (Issa et al. 2005). This possible adverse effect of dental amalgam is widely recognized and reflected in contemporary contra-indications for the use of this material. Burning Mouth Syndrome can occasionally be associated with a change in the appearance of the clinically normal oral mucosa. In some case it may be associated with a strong allergy to mercury and a positive patch test supports the removal of the amalgam filling. Full recovery and complete remission of systemic dermatitis may occur after removal of a mercury-containing filling (Pigatto et al. 2004). Patch-test analysis for the determination of mercury allergies was carried out by Wong &Freeman (2003) on a group of 84 patients with reticulate, lacy, plaque-like or erosive oral lichenoid lesions. Thirty three (39%) of the patients had positive patch test findings. The amalgam fillings were removed for thirty of these, and an improvement was seen within 3 months in 28 of these (87%).
3.3.6.2. Systemic reactions
General
There are some epidemiological studies on the health effects of mercury released by dental amalgam fillings. The effects reported may affect the nervous and renal system, and also the immune, respiratory, cardiovascular, gastro-intestinal, haematological, and reproductive systems. Bates (2006) reviewed these studies and concluded that the available studies show little evidence of effects on general chronic disease incidence or mortality.
Reports of effects caused by amalgams have involved many diseases. A few data suggest that the mercury from amalgam reduces lymphocytes responses, compromising immune functions. As a consequence, amalgam has been implicated in the development of Alzheimer’s disease and there is a long list of heterogeneous diseases that might be due to the accumulation of mercury in the body. However, for many of the claims, scientific investigations have tended to provide either refutation or evidence of a lack of correlation. There is usually little evidence of general chronic disease incidence or mortality associated with dental amalgams. In one New Zealand retrospective cohort study of 20.000 military personnel (84% males) followed up for 20 years, data on dental history was linked with national mortality, hospital discharge and cancer incidence databases. There was no association between dental amalgams and chronic fatigue syndrome or kidney diseases. The number of cases for investigation of Alzheimer’s or Parkinson’s diseases was insufficient to draw any conclusion (Bates et al. 2004).
No link has been detected between mercury exposure and negative health effects with respect to dentist mortality, although the mercury blood level is higher in dentists than in a control population. The life span of dentists was shown to be three years greater than that for a control non-dentist group. The same type of effect was seen with many other parameters, indicating that the general health of dentists is good (McComb 1997).
In several situations, such as with Alzheimer’s and Parkinson’s diseases, there is no definitive answer concerning causation and caution has to be expressed, bearing in mind that this collection of diseases possibly associated with amalgam restorations bears little comparison with the known characteristics of the occupational toxicology of mercury.
The available evidence is discussed here in relation to specific organ systems.
Urinary system
A few studies have investigated the relation between amalgam and kidney function. Except for a small increase in N-acetyl-Î2-glucosaminidase, which is not considered to have any clinical significance, no parameters suggest that there is an association between amalgam fillings and kidney diseases. Evidence of renal disease was investigated among dentists, who are exposed to greater levels of mercury vapour than other populations, but no kidney dysfunction has been found. During on-site screening of dentists at annual American Dental Association meetings in 1985 and 1986, the mean urinary values were of mercury were 5.8- 7.6 µg /l , showing that dentists have a much higher mean urinary mercury, but there was no evidence that they exhibited any higher levels of morbidity, mortality and kidney dysfunctions (see for review: Dodes 2001). It is recognized that mercury does induce antinuclear antibodies and the induction of metal- associated autoimmunity in general, with some effects in the renal system (Bigazzi 1999).
Bellinger et al. (2006), in a comprehensive neurophysiological and urological analysis of 534 children followed for five years in a randomized clinical trial, comparing groups with amalgam restorations and alternative composite resins. There were no statistically significant differences between these two groups in renal glomerular function as measured by creatinine adjusted albumin levels.
The overall conclusion of the epidemiological studies suggests that there is no evidence that dental amalgam fillings affect kidney function in human.
Neurological System
Alzheimer’s Disease
Inorganic mercury is a neurotoxin at high doses and it has therefore been suspected to play a role in the pathogenesis of neurodegenerative diseases such as Alzheimer’s disease. Mercury vapour released by dental amalgam has been suspected of being one of the potential factors relating to this disease. However, when autopsies of subjects with and without Alzheimer’s disease were carried out, no significant association of the disease with the number, the surface area or history of dental restorations was found. Retrospective cohort studies provide limited evidence of an association between amalgam and this disease (Bates et al. 2004). There was no significant difference in brain mercury levels between Alzheimer’s disease and control subjects (Saxe et al. 1999).
Multiple Sclerosis
Although a few articles have concluded that there is some suggestion of a possible association between amalgam and multiple sclerosis, the evidence is inconclusive. A systematic review and meta-analysis suggests that there is a non-statistically significant difference in the risk of multiple sclerosis between individuals with and without amalgam restorations. However, the small number of subjects, inadequate exposure data, and inadequate control recruitment methods constitute limitations of the available studies. Without any knowledge on the size of the restoration, the surface area, the duration of the exposure, it is not possible to confirm or to rule out any link between amalgam and multiple sclerosis (Aminzadeh and Etminan 2007).
One case control comparison between 132 multiple sclerosis patients and 423 controls failed to demonstrate an association between the number of dental fillings, the duration of the exposure to dental amalgam and the condition (Casetta et al. 2001). However, in one further study a correlation was found between the number of amalgam restorations in the a multiple sclerosis group of 39 females compared to matched 62 controls, although it is impossible to establish any temporal relationship concerning cause and effect in such a situation; in other words it may not be possible to determine whether patients with such a neurological condition are more likely to need dental restorations because of difficulty with oral hygiene (McGrother et al. 1999). In another case-control study (Bangsi et al. 1998) a comparison was made between 143 multiple sclerosis patients and 128 controls, where neither the number nor the duration of exposure to amalgam fillings supported an increased risk of multiple sclerosis.
Parkinson’s Disease
Parkinson’s disease involves the aggregation of alpha-synuclein forming fibrils, the major constituent of intracellular protein inclusions (Lewy bodies and Lewy neurites) in dopaminergic neurons of the substantia nigra. Aluminium, copper, iron, cobalt and manganese are effective di- and trivalent metals that may be involved in this process; however mercury is also included as a risk factor. Even low concentrations of some metals can directly induce alpha-synuclein formation (Uversky et al. 2001). An analysis of 130 patients with confirmed disease versus matched controls support the view that the disease has a multifactorial etiology, involving genetic, environmental, trauma, and possibly other factors (Semchuk et al. 1993). Consequently, it is very difficult to establish any causal link with a putative agent such as dental amalgam. In one study, occupational mercury exposure was related to an eightfold increase in risk of Parkinson’s disease (Schulte et al. 1996), but this is still a matter of debate and there is no scientifically sound report establishing a direct relation with dental fillings.
Paresthesia
Paresthesia is considered to be the most sensitive neurological effect, and is produced by blood mercury concentration in the range of 34 to 97µg/l. A deficit in neurocognitive functions may result from doses below those considered to be the threshold for general clinical effects. Accentuated postural tremor, impaired coordination, positive Romberg sign, and reduced distal sensation suggesting peripheral neuropathy have been reported especially among those occupationally exposed to mercury. Low-dose, long-term exposure to mercury vapour from dental amalgam has been suggested as a risk factor. However, Kingman et al. investigated the relation between amalgam exposure and neurological functions in a cohort of 2038 participants (Kingman et al. 2005). No significant trends between neurological signs (tremor, alternate motion rate, coordination, vibrotactile threshold deficit, proximal and distal strength and station) and the presence of dental amalgam were detected. Therefore, no link could be established between peripheral neuropathy and amalgam exposure.
Autism
Mercury and an infectious agent such as the measles virus may contribute to the immunopathogenesis of autism (Cohly and Panja 2005). Studies showing elevated brain specific antibodies support an autoimmune mechanism. A virus may initiate the process but subsequent activation of cytokines is the damaging factor associated with the disease. Environmental exposure to mercury is suggested to modulate immune homeostasis. These hypotheses have not yet been demonstrated, but their involvement in autism cannot be ruled out (Cohly and Panja 2005). Some data are related to the possible effects of the mercury-containing Thimerosal, included in certain vaccines to protect from bacterial and fungal contamination. One retrospective cohort study did not support the possibility that Thimerosal exposure causes neurodevelopmental disorders (Andrews et al. 2004). The systematic critical review of the articles published between 1966 and 2004 does not support any relationship between the mercury-containing vaccine and clinical findings (Parker et al. 2004). A report for the Food and Drug Administration by the Institute of Medicine (IOM 2004) confirms that no link has been yet established between vaccines, Thimerosal and autism. There is no evidence of a causal relationship between dental amalgam and autism.
Amyotrophic Lateral Sclerosis
There is no evidence for a relationship between Amyotrophic Lateral Sclerosis (ALS) and mercury. A retrospective case-control study was conducted on 66 ALS patients and 66 age- and sex-matched control patients. No association was found between heavy metal exposure and the pathogenesis of ALS (Gresham et al. 1986).
Psychological Conditions
During the past two decades, mercury and heavy metals have been claimed to be responsible for a series of mental health problems, with a variety of symptoms. Between 1978 and 2007, a total of 53 publications in international journals were published and listed in MedLine, with an increased tendency to take into account the psychological and psychiatric aspects of these patients. However, evidence is lacking for a causal link between mercury and human mental health problems or psychological conditions.
A series of self-assessed patients were referred to the Dental Biomaterials Adverse Reaction Unit in Bergen, Norway (Lygre et al. 2005). Patient’s complaints were heterogeneous. Many individuals displayed multiple subjective symptoms associated with several organ systems. The most common were fatigue, muscle and joint pain, dizziness and headache. Intra-oral symptoms were related to burning sensations, taste disturbances and dry mouth. After removal of the mercury-containing fillings, a small decrease in the intensity of different symptoms was noted. Intra-oral symptoms were decreased and the decrease was statistically significant for taste disturbances (p=0.001), dry mouth (p=0.034), and stiffness/paresthesia (p=0.05). However, the symptoms were still higher than in a reference group sampled from the general population in Norway.
A psychiatric diagnosis was established in 70% of the patients referred for self-reported complaints, which they had attributed to amalgam restorations; this compared to 14% in the control group. The prevailing symptoms were anxiety, asthenia and depression. Mercury levels were similar in the two groups, and far below the critical levels of mercury intoxication. No positive patch test was found in any of the two groups. As the number of fillings and the mercury level were similar in the two groups, the authors concluded that mercury was not the cause of the impaired health reported by the patients, and that the reported symptoms were parts of a broad spectrum of mental disorders (Bratel et al. 1997a,b).
The psychological/psychiatric, odontological and medical aspects of patients with symptoms attributed to the side effects of mercury-containing dental filings were studied in a total of 67 patients and 64 controls matched for age, sex, and residential area. The high prevalence of psychiatric disorders (89% in the patient group) compared to the control group (6%) seems to constitute the main characteristic of the patients. The clinic and medical data did not provide any explanation on the occurrence of the symptoms (Bagedahl-Strindlund et al. 1997).
General neuropsychological and neurophysiological functions
One epidemiologic study showed no evidence of deterioration of performance associated with amalgam exposure. The evaluation of relationships between amalgam fillings and any decrease of peripheral neurological function did not allow any correlation to be established. The mouths of 2038 US military personnel were examined, the number of oral fillings scored and neurological function assessed (Kingman et al. 2005). Consistent with other studies, no evidence of effects of amalgam fillings on neurological functions was found.
Another study (Factor-Litvak et al. 2003) was carried out on 550 adults, aged between 30 and 49 years. Urinary mercury was 1.7µg/gC (range 0.09-17.8), the mean number of amalgam surfaces was 10.6 (range 0-19). It was concluded that mercury exposure derived from dental amalgam was not associated with any detectable deficit in cognitive or fine motor functioning.
While many individuals consider that their neuropsychological conditions are related to exposure to dental amalgam the literature contains no credible supportive data
Psychological Development
Two randomized, controlled clinical trials have been carried out on the neuropsychological and renal effects of dental amalgam in children (Bellinger et al. 2006 and 2007, DeRouen et al. 2006). In the first study 534 children aged 6 to 10 years living in New England area (USA), were randomly assigned to receive dental restorations using either amalgam (n=267) or resin composites (n=267). They were examined after a 5- year period. No difference appeared in full-scale IQ. No difference was found in the general memory index. Over the 5-year period, a significantly higher mean urinary mercury level was noted, but no renal effect was observed (Bellinger et al. 2006). The latest publication from this group (Bellinger et al. 2006), concludes that the exposure to mercury from dental amalgam was not associated with any adverse neuropsychological effects over a five year period and that the use of dental amalgam is not associated with an increase in children’s risk of experiencing neuropsychological dysfunction. Another randomized clinical trial with annual follow-up for 7 years was carried out on 507 children in Lisbon, Portugal. The children received either amalgam restorations (n=253) or resin composites (n=254). The creatinine-adjusted urinary mercury levels were 1.8µg/g in the amalgam group, and 1.9µg/g in the composite group. No statistically significant difference was found in measures of memory, attention, visual function, or nerve conduction velocities over all the 7 years of follow-up. The authors noticed also that the need for additional restorative treatment was approximately 50% higher in the composite group. These data suggest that exposure to dental amalgam restorations within this age range has no effect on psychological development, with the superior performance of the amalgams compared to alternatives being noteworthy, although of course each procedure with a non-amalgam alternative would normally be less invasive.
As noted above, epidemiological evidence supports the view that low-level mercury exposure is not a cause of autism. Based on a recent meta-analysis, from all the published data, the risk of neurodevelopmental disabilities from low-level methylmercury exposure has not been established (Ng et al. 2007).
There is evidence of in utero exposure of mercury to the fetus, or in infancy through the breast milk transfer. The relationship between mercury exposure from dental filling placement during pregnancy and low birth weight risk was investigated on a cohort of 1117 women with low-birth weight infants (< 2.500 g) compared with 4468 women with infants weighting 2.500g or more. The study found no evidence that the mercury- containing dental fillings placed during pregnancy increased low-birth-weight risk (Hujoel et al. 2005).
It has already been noted that mercury is able to induce autoimmunity in susceptible strains of rodents and so the question arises as to whether such effects are seen in humans with respect to amalgam related mercury exposure. In man a correlation between plasma mercury and IgE levels has not been demonstrated, while contradictory results have been seen with other immunoglobulins (Langworth et al. 1993, Queiroz et al. 1994, Herrström et al. 1994, 1997). No association was found between the number of fillings in individuals and Henoch-Schönlein purpura and acute glomerulonephritis, which are all autoimmune diseases. With respect to the reduced lymphocyte responses, Mackert et al. (1991) showed no indication that amalgam affects the human immune system. Epidemiologic studies have shown that occupational exposure to mercury does not usually result in autoimmunity.
Mercury does induce antinuclear antibodies, scleroderma-like diseases, lichen planus, or membranous nephropathy in some individuals. Immunogenetic and pharmacogenetic factors are responsible for the induction of metal-associated autoimmunity in general (Bigazzi 1999). In addition to estrogen replacement therapy, other factors including mercuric chloride are putative risk factors for the development of lupus, scleroderma, and Reynaud disease. Mercuric chloride causes complex glomerulonephritis and autoantibodies recognizing a nucleolar protein, fibrillarin. Antibodies directed against fibrillarin are higher in scleroderma patients. Urinary mercury excretion has been reported to be higher in scleroderma patients who are positive for antifibrillarin antibodies. However this level is still in the normal and unexposed ranges, and these patients never develop immune complex glomerulonephritis (Mayes 1999).
Another epidemiological study established that the effects of mercury occur at high doses which are above the levels to which humans would be exposed through fish consumption. The hypothesis was tested that mercury exposure does not cause autoimmune disease directly, but rather interacts with genetic predisposition, or with exposure to antigens or infection, and consequently exacerbates the disease, acting as a co-factor (Silbergeld et al. 2005).
As mentioned above, mercury like other metals is well known for its potency to induce allergic contact dermatitis (Garner 2004, Khamaysi et al. 2006). Indeed a high percentage of patients with localized mucosal reactions (oral lichen planus) shows a positive skin patch test for amalgam or mercury and removal of dental amalgam restorations can result in clinical improvement and even complete remission (see 3.3.6.1).
Reproductive system
Although reproductive effects have been addressed in several of the studies discussed in this Opinion, there is very little data available on this subject. There is no evidence of any association between amalgam restorations and either male of female fertility or obstetric parameters. One study that attempted to examine the question of fertility in detail failed to show any correlation between the mercury burden from amalgam restorations and male fertility disorders (Hanf et al. 1996). No evidence can be found for any relationship between amalgam restorations and birth defects.
Miscellaneous effects
The risk of coronary heart disease in man was studied in 470 cases of coronary heart disease (coronary and artery surgery, non fatal myocardial infarction, and fatal coronary heart disease). The mercury level was significantly correlated with fish consumption, and the level of mercury higher in dentists than in non-dentists. However, the mercury level was not associated with the risk of coronary heart disease (Yoshizawa et al. 2002). However, in a further study of a birth cohort, methylmercury exposure was associated with decreased sympathetic and parasympathetic modulation of the heart rate variability (Grandjean et al. 2004).
Long-term parenteral exposure to mercury may occur in patients with hypogammaglobulinaemia. The patients receive regular long-term replacement therapy with a concentrate of pooled human immunoglobulin G containing an organic mercury compound (Thiomersal) as a preservative. In 26 such patients, the urinary mercury level ranged from 4 to 734mg (mean 152mg) over treatment periods of 6 months to 17 years (mean 6.5 years). The urine concentration was raised in 73%, but without any correlation between urine mercury and the age of the patient, the IgG dose, or the duration of the treatment. No clinical evidence of toxicity was apparent (Haeney et al. 1979).
At the present time we may conclude that there is no epidemiological evidence to support the contention that mercury released by dental amalgam fillings contributes to the etiology of systemic diseases.
3.3.7. Epidemiological and clinical evidence concerning adverse effects of dental amalgam in dental personnel
As with individuals with amalgam restorations, adverse effects of mercury exposure in dental personnel have been the subject of numerous investigations (Hörsted-Bindslev 2004). These investigations have focussed on general reactions to chronic low-level exposure to mercury and atypical mercury body burden.
Jones et al. (2007) reported possible residual adverse effects from occupational mercury exposure in dentistry, Thirty years ago, the all-women exposed group worked with both silver and copper amalgam filling material without protective gloves or a ventilation system, resulting in chronic mercury exposure. The aim of the study was to test the null hypothesis in a survey of general and reproductive health, and a battery of nine neurobehavioral tests. The population was the 115 graduates of one school for dental nurses from 1968 to 1971. The sample was 43 mercury-exposed women and 32 matched controls. Statistical comparisons revealed that the two groups were equivalent on cognitive tasks and four of the six mood subscales. Significant between-group differences were found in current health symptom experience and reproductive health, especially early hysterectomy experience.
Concerning neurobehavioral studies, the review of Hörsted-Bindslev (2004) determined that it was justified to conclude that a risk of subtle neurotoxic changes may occur in dental personnel, who show a urine concentration of mercury below that which is seen when operating within the accepted threshold limit. However, they stressed that other factors such as the daily exposure to high frequency vibrations (Åkesson et al. 1995) and stress may be equally important for the subtle behavioural changes. Also none of the studies referred to had shown the dental personnel to suffer the classical signs of mercury intoxication. This conclusion is mirrored by others: for example the principal conclusion of Ritchie et al. (2002) indicated that although differences in health and cognitive functioning between dentists and controls could be found, these differences could not be directly attributed to their exposure to mercury. They further recommended that environmental monitoring of dental surgeries should be regularly conducted to ensure that dental personnel were not exposed to mercury concentrations above the occupational exposure standard. The need for such measures will diminish with further reductions in the use of dental amalgam and fewer amalgam restorations being removed in everyday clinical practice. The possible exception may be dental personnel with a brain-derived neutrotrophic factor (BDNF) polymorphism which may be associated with abnormal intracellular trafficking in hippocampal neurons which, in turn, may be associated with episodic memory impairment, as described by Echeverria et al. (2005). Non-neurological adverse effects of occupational exposure to mercury have been claimed to be many and varied, in a similar fashion to those alleged to occur in patients. Of particular concern to dental personnel have been the possible reproductive effects of occupational exposure to mercury. In contrast to the work of Rowland et al. (1994) which reported that chair-side assistants with a high occupational exposure to mercury were less fertile than unexposed controls, a substantial study in Norway by Dahl et al. (1999) found no difference in fertility between high school teachers and dental surgeons, of whom one-third placed more than 50 restorations of dental amalgam a week. Work by Lindbohm et al. (2007) found a slightly increased risk of miscarriage amongst “dental workers” with occupational exposure to dental amalgam, but no pattern of dose-response was found. Lindbohm et al. (2007) concluded that no strong association or clear dose- response relationship could be observed between occupational exposure to chemical agents or restorative materials (including dental amalgam) and the risk of miscarriage amongst dental personnel. It was acknowledged, however, that the possibility of a slightly increased risk of miscarriage among exposed workers could not be excluded. Concerning cytogenetic damage in dentists exposed to mercury, Atesagaoglu et al. (2006) found that examination of leukocytes from dentists exposed to mercury vapour below concentrations of 0.1mg/m3 failed to reveal cytogenetic damage.
3.3.8. Life-cycle of mercury in relation to dental amalgam
This Opinion is concerned with the possible direct effects on human health arising from the use of amalgams, relating both to patients and dental
personnel. There is an obvious life cycle for the mercury used in these amalgams. This starts with the opening of a packaged amalgam product in the dental clinic, followed by its clinical handling during placement and possible subsequent manipulation or removal, the possible excretion or exhalation of mercury from recipients throughout their lifetime, and culminates with the disposal of the body. Implicit in this life cycle is the exposure of the environment in general and the possibility of indirect effects on human health in general. The detailed discussion of these life cycle factors and environmental effects is outside the scope of this Opinion. It is noted, however, that amalgam waste management, including the disposal of packaging materials and surplus amalgam is take seriously in the dental profession with respect to dental clinics and offices (Jokstad and Fan 2006) and detailed studies have recently been performed on the mercury generation from dental waste amalgam and its potential for both recycling and environmental exposure (Drummond et al. 2003). With respect to disposal of amalgam-containing bodies, no significant information can be found about contamination at burial sites, but it is known that cremation process will yield mercury emissions (Santarsiero et al. 2006). These have been estimated to range from 0.036 to 2.140 g mercury per corpse, with mercury concentrations ranging from 0.005 to 0.300 mg/m3.
3.3.9. Experience with non mercury-based fillings/amalgams
Mercury is not the only element that is liquid at room temperature and some others have also been considered for use in dentistry. As reported by Hero and Okabe (1994), gallium has been in use, in limited amounts, since 1956, but they did note problems with corrosion resistance and overall biocompatibility. Dunne et al. (2005) have recently published a longitudinal controlled clinical study of a commercially available gallium based restorative material and found the clinical performance so grossly inferior to a control amalgam that its continued clinical use could not be justified. Indium has also been considered, but mostly as an adjunct to mercury, possibly replacing up to 10% of the mercury, but there is little evidence about either performance or safety (Johnson et al. 1992) and its use is not considered significant.
3.3.10. General Observations on Amalgam Efficacy
The efficacy, longevity and general performance of amalgam restorations has been assessed on many occasions in the past, and it is not necessary to review these studies here. Whatever the material chosen, direct restorations may fail, primarily through secondary caries, fracture of the restoration or tooth, marginal deficiencies or wear. The rates at which these failures occur are difficult to compare since they will vary with clinical technique and patient characteristics, and since there have been improvements to the quality of all materials over time. It remains the view, however, that from mechanical functionality and longevity perspectives and resistance to secondary caries, possibly through anti-bacterial activity, amalgam will outlast alternative materials under many circumstances (Mitchell RJ et al. 2007). From such perspectives, it may still be the material of choice with many dental practitioners for large restorations and the replacement of large restorations. It is with respect to their aesthetics and non-adhesive character, which means that larger cavities have to be prepared, often with excessive tooth tissue removal, that amalgams may be seen to be inferior to the alternatives, and it is this, and not overall longevity, that is driving a change to these alternatives.
3.3.11. Conclusions on Dental Amalgam
We emphasise that dental amalgam remains an effective restorative material and, from the several perspectives of performance and economics, may be considered the material of choice for some restorations in posterior teeth. However, because dental amalgam is not tooth-coloured nor does it adhere to remaining tooth tissues, its use has been decreasing in recent years and tooth-coloured filling materials have become increasingly more popular, consistent with the general trend towards more minimal intervention techniques in dentistry. There has been for some years a move towards non-amalgam, adhesive, tooth coloured restorations. This trend shows some variations within and between countries, and is emphasized by the significant reduction of training in the placement of dental amalgam restorations and the corresponding increase in training in the use of amalgam alternatives in a growing number of dental schools. We anticipate there to be a continued and sustained reduction in the use of dental amalgam in oral health care provision across the European Union, the rate of which is dependant on trends in dental education towards the increasing use of alternative materials in place of amalgam and the possible reduced availability of mercury products in general.
It is recognized that mercury which is the major metallic element used in dental amalgam, does constitute a toxicological hazard in general, with reasonably well defined characteristics for the major forms of exposure. It is accepted that the reduction in use of mercury in human activity would be beneficial, both for the general decrease in human exposure and from environmental considerations.
However, with respect to the debate about the possibility of causal relationships between the use of mercury containing amalgam and a wide variety of adverse systemic health effects and taking into account many studies and investigations into this putative causal link, there is no unequivocal evidence to support this possibility. These studies have included assessments in children and in pregnant and lactating women. It is generally concluded that no increased risks on adverse systemic effects exist and we do not consider that the current use of dental amalgam poses a risk of systemic disease. It is recognized that some local adverse effects are occasionally seen with dental amalgam fillings, but the incidence is low and normally readily managed. It is also recognised that there have been reports of reactions to dental amalgam, which are not supported by scientific evidence, but indicate that very occasionally an individual may have unexplained atypical physical or other reactions attributed to mercury.
The main exposure to mercury in individuals with amalgam restorations occurs during placement or removal of the fillings. The transient mercury release during placement and removal will result in exposure to the patients and also to the dental personnel. It should be noted that the removal of amalgam restorations will result in a scute relatively high exposure of the individual patient to mercury compared to leaving the amalgam filling intact. We find no evidence of clinical justification to remove clinically satisfactory amalgam restorations with the exception of those patients which are suspected to have allergic reactions and positive patch tests.
Source & ©: SCENIHR,
![]()

This summary is free and ad-free, as is all of our content. You can help us remain free and independant as well as to develop new ways to communicate science by becoming a Patron!